Community Health Workers and Urban Communities
Nearly half of the world’s population lives in urban areas4, yet many of the individuals who live in them face significant barriers that impact their health. Often referred to as the social determinants (of health), factors such as affordable housing, unemployment, health care access or affordability, and economic status create health disparities for the individuals that live there.9
Community Health Workers and Urban Communities
Nearly half of the world’s population lives in urban areas4, yet many of the individuals who live in them face significant barriers that impact their health. Often referred to as the social determinants (of health), factors such as affordable housing, unemployment, health care access or affordability, and economic status create health disparities for the individuals that live there.9
Community Health Workers Improve Health Outcomes
The success of Community Health Worker (CHW) programs have had improving health outcomes for individuals living in rural communities by providing services such as health education, referrals to resources, social support groups, and health insurance application assistance is well documented. Although the design and implementation of these programs can change, the services CHWs provide also play an important role in assisting individuals that live in urban settings.1
What is unique about CHW programs is that they address social barriers from a perspective of health. Because CHWs come from and understand the languages of the communities in which they serve, they have personal insight on how social factors impact their community’s health. This understanding allows them to build trust with residents, which in turn gives CHWs the ability to disseminate health information effectively. CHWs also have access to locations where their community members live, work, worship, and seek services. This access allows them to coordinate and strategize the most effective outreach methods. In other words, CHWs know their community and know how to talk to their community members in a way that empowers them to take actionable steps.
Community Health Worker Programs Address Health Challenges in Cities
Urban populations live in communities often characterized as having a high population density, unplanned development, and population demands that often exceed service capacity. 2 These communities can represent a diverse group of people around the world, and in the U.S., they are often made up of people of color or individuals who have recently immigrated to the country. Despite geographic and demographic differences, rural and urban populations share similar barriers to health such as high rates of diabetes and chronic conditions, higher rates of uninsured individuals, and access to affordable and culturally identifiable services.6
Diabetes
Racial and ethnic minorities that live in or around cities represent about two-thirds of individuals with diabetes globally.7 While social and cultural factors still play a role in the prevalence of diabetes in urban areas, the convenience of travel (think mass public transportation), the reduced physical demand required to provide food, and the increased availability of low-cost, highly processed foods contribute to the promotion of diabetes in this setting.7 This is why CHWs expertise in outreach and health education is crucial. CHWs know where and how community members purchase their foods and build relationships with these establishments to collaborate on initiatives.
For example, a study of the program, Vida Sana Hoy y Mañana (Healthy Life Today and Tomorrow), used Community Health Workers to promote the consumption of fruits and vegetables inside local Hispanic focused grocery stores often referred to as bodegas. The study found that individuals in this store reported an increase in fruit and vegetable consumption by about one additional serving per day.16
Community Health Workers are also great at group facilitation which allows them to educate large groups of people at once, on topics that have implications for diabetes and other chronic conditions. An example of this is the Harlem Health Advocacy program in New York City. CHWs conducted outreach and provided health coaching to individuals that lived in public housing complexes and senior centers. The results of the program found that 94% of participants continued to stay active for at least 6 months and blood pressure control increased significantly.15
Affordable Health Care Coverage
In the U.S., overall, residents in rural populations are less likely to have private health insurance than those in urban areas.11 However, factors such as affordability, unemployment, and misconceptions about the health care system still leave many individuals who live in urban settings without coverage. In many cities in America, the unemployment rates are higher for blacks and Hispanics that live in and around large cities.8 This means that a large part of this population is without employer-based coverage or cannot afford private insurance.
Because Community Health Workers serve as a bridge between health care systems and the communities they come from, they know what low-cost or free services are available at a local and federal level. They can provide education to individuals in the language they are comfortable with which is a big help when it comes time to dispel myths on the health care process. These skills also allow CHWs to help individuals with the application process. They can promote open enrollment periods, deadlines, and requirements in a way that their population can understand.
Access to Services
Like in rural areas, urban populations face challenges when trying to locate and access services they can identify with culturally. African Americans, Hispanics, and Native Americans account for nearly one-third of the population but only represent 9% of physicians, 7% dentists, 10% of pharmacists, and 6% of registered nurses.5,12 This is why CHWs use their trusting relationships with community members to build stronger connections between individuals and their health care providers. This trust allows for a more effective exchange of information between provider and client.
Further, CHWs consider more than just an individual’s medical needs. They work with community partners to address the social and economic barriers that prevent people from getting the help they need. For example, a CHW will know if an individual does not have bus or train fare to make it to a medical appointment and can connect them to organizations that cover these fares for qualifying individuals. Understanding small details such as this is what sets CHWs apart from other health professionals and what allows them to minimize barriers individuals face when seeking services.
Community Health Workers Improve Health Outcomes
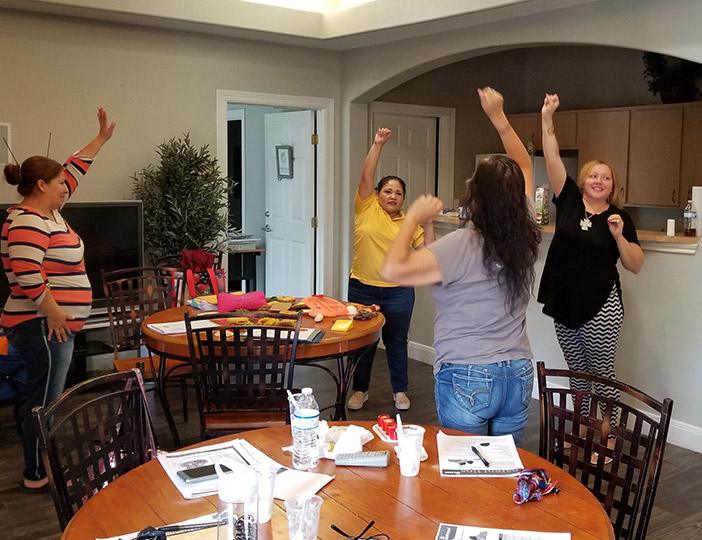
A CHW leads low-impact exercises individuals can do in their own homes.

CHWs teach healthy eating habits using unique tools catered to the culture of their community, such as food models and plastic portion plates.
The variety of work CHWs perform allows for flexibility in the way organizations implement CHW programs in their communities. Because CHW programs can be tailored to fit the needs of specific populations, definitions within the profession vary. Although variations exist, there are key themes shared across all of the ways CHWs are described. MHP Salud has compiled these themes and used over 35 years of experience implementing CHW programs to define Community Health Workers as…
a trusted member of the community who empowers their peers through education and connections to health and social resources.
In urban areas, there are a variety of health professional positions that share similar qualities of Community Health Workers. For example, Health Educators and Outreach Workers are titles used to describe health professionals who provide health information and education. Healthcare Workers and Navigators may be used to describe CHWs that focus on connecting individuals to health care services. These positions share a similar responsibility with CHWs, to serve as a bridge between the health care system and the community.
However, what makes CHWs unique is that they must be a member of the community they are serving. This qualification means that CHWs are equipped with a deep understanding of the cultural norms and practices within their community. They can use this understanding to strategize the use of the most effective methods to perform the duties of their role.
Our CHW Programs in Tampa and Orlando

Aprendiendo Lecciones del Arte de Sobrevivir (Learning Lessons on the Art of Survival) is a Promotora (Community Health Worker)-led program that aims to establish a network of peer support for Latino(a) survivors of sexual assault and offers participants opportunities to share their experiences and perspectives with other survivors.

A woman decorates a personal journal as an activity in El Arte de Sobrevivir
MHP Salud implements CHW-led programs in predominantly Hispanic urban communities in the Tampa and Orlando region of Florida, on the topic of Healthy Relationships. These programs provide information, resources, and support to survivors of domestic violence, intimate partner violence, and sexual assault. Although many individuals are victims of these crimes, Latinas face unique challenges.
50% of Latinas who experience abuse never report it to authorities due in part to the fact that Latina survivors prefer to talk with trusted family members and friends.13,14 The nature of the relationship between CHWs and those they serve through our Healthy Relationship programs allows them to fill the role of that trusted member. CHWs also had established connections with local organizations and groups which helped identify individuals who needed services and offered safe spaces for groups to meet. These collaborations are crucial in urban areas where resources are often limited because of high demand. Further, they help establish a continuum in which CHWs can refer individuals to services that are available within the same space of the program.
These programs demonstrate that whether CHWs implement programs in rural or urban settings, the services they provide are crucial in connecting communities that face barriers to health to the services they need.
- https://academic.oup.com/heapol/article/35/1/91/5607274
- Vlahov D, Freudenberg N, Proietti F et al. Urban as a determinant of health. Journal of Urban Health 84: 16–26. https://link.springer.com/article/10.1007/s11524-007-9169-3
- https://srhrc.tamhsc.edu/docs/chw-policy-brief.pdf
- https://www.who.int/health-topics/urban-health
- http://urbanuniversitiesforhealth.org/media/documents/Fact_Sheet_on_Health_Disparities_and_Urban_Health_Workforce.pdf
- Cyr, M.E., Etchin, A.G., Guthrie, B.J. et al.Access to specialty healthcare in urban versus rural US populations: a systematic literature review. BMC Health Serv Res 19, 974 (2019). https://doi.org/10.1186/s12913-019-4815-5
- http://www.citieschangingdiabetes.com/content/dam/cities-changing-diabetes/magazines/CCD-briefing-book.PDF
- https://www.brookings.edu/blog/the-avenue/2019/06/26/black-workers-are-being-left-behind-by-full-employment/
- https://www.who.int/bulletin/volumes/88/4/10-010410/en/
- https://www.census.gov/library/visualizations/interactive/rural-urban-uninsured.html
- http://nciom.org/rural-urban-uninsured-gap-persists-but-more-north-carolinians-have-insurance/
- https://www.pewsocialtrends.org/2018/01/09/diversity-in-the-stem-workforce-varies-widely-across-jobs/
- https://www.decimosnomas.org/wp-content/uploads/4.16-NO-MAS-STUDY-media-findings-FINAL-FINAL-updated-Avon-logo-11.16.15.pdf
- Cuevas, C.A., K.A. Bell, and C. Sabina, Victimization, psychological distress, and help-seeking: Disentangling the relationship for Latina victims. Psychology of Violence, 2014. 4(2): p. 196-209. https://psycnet.apa.org/record/2014-12472-003
- https://www.cdc.gov/pcd/issues/2019/18_0623.htm
- https://www.ncbi.nlm.nih.gov/books/NBK208027/
Promotora de Salud Resources
In order to do their complex work, Promotores and Promotoras must possess or build communication and interpersonal skills to conduct effective outreach in their communities. In addition, they must develop the skills to facilitate educational sessions and be able to coordinate assistance from many different resources to many different individuals who understand information better when it is in Spanish. And due to the sensitive nature of some of the issues they address; Promotores and Promotoras need personal strength as it’s possible that they’ll be working with individuals they already have relationships with.
It is crucial that Promotores and Promotoras feel supported in their unique roles. MHP Salud has used over 35 years of experience to develop free resources to help Promotores and Promotoras de Salud strengthen and increase their skills, and resources to help Supervisors and Managers support them.
Sign up for our free resource portfolio which includes educational items such as:

About MHP Salud
MHP Salud provides opportunities to organizations interested in the Community Health Worker (CHW) profession to grow their knowledge base on how to design, implement, and evaluate CHW programs for their populations. We offer training for CHWs, CHW Supervisors, along with professionals and grant writers working with CHW programs. We also offer CHW program consulting and guided implementation packages that can be tailored to meet the needs of any organization. Our services are affordable and available both in-person and virtually. Learn more by visiting our CHW Training and Consulting page.




