MSAW and Latino Communities Managing Diabetes
Published September 2021 | Back to all news and updates.
Diabetes affects Americans of all socioeconomic statuses, races, cultures, and ethnicities. However, Hispanic/Latinos are at higher risk of having type 2 diabetes as compared to other ethnic groups. Migrant Seasonal Agricultural Workers (MSAWs) are predominately of Hispanic/Latino descent placing them at higher risk for type 2 diabetes. MSAWs may be vulnerable to this condition as a cause of several factors such as working and living conditions, poverty, migratory status, and lack of resources. Diabetes is a chronic illness that causes more blindness, kidney failure, and lower-limb amputations than any other single disease. (1)
Underserved communities, including MSAWs, may lack resources and health insurance to be screened, diagnosed, and/or treated for diabetes. This may be due to their fear of accessing medical care because of their immigration status and/or there may be a lack of services in their preferred language. MSAWs are constantly migrating for work, which interrupts continuous care and follow-ups. MSAWs may also lack access to affordable, nutritious food, causing them to choose unhealthy, processed food which can lead to obesity. Additionally, the high cost of diabetes management supplies and medication, and stigmas related to diabetes can lead to poor outcomes for MSAWs dealing with diabetes. In the Hispanic/Latino culture, the stigma around diabetes is correlated with the idea that illness is sometimes seen as a sign of weakness. Hispanic cultural norms around food can create barriers to making changes related to diet and exercise; being underweight is seen by some as a sign of illness, whereas being overweight is seen as healthy. (2). For MSAWs with diabetes, it can also be challenging to incorporate lifestyle changes that affect other family members, especially if family members are hesitant to adapt to new foods or to incorporate more physical activity.
MSAWs work long hours, outdoors, often in hot temperatures, and around heavy machinery. Their working conditions can affect their diabetes management in many ways such as not having access to medication storage and proper hydration. MSAWs can prevent injury while working out in the fields, on muddy grounds, around heavy machinery, or near animals by wearing protective footwear such as steel-toe/steel shank shoes which provide foot support and help distribute weight evenly. Injury can result from an animal stepping on its feet and/or heavy and sharp objects penetrating a shoe. (3) Although there are many health considerations when managing diabetes, MSAWs often overlook the importance of taking care of their feet.
Diabetes Foot Care
The lack of foot care can be dangerous to a patient with diabetes as this can lead to serious foot complications including injuries, nerve damage, and amputations. Diabetic neuropathy is a type of nerve damage that occurs in patients with diabetes. This is caused by high blood sugar which can injure nerves throughout your body and often damages the nerves in the legs and feet. (4) Diabetes nerve damage causes loss of feeling, numbness, and/or reduced blood flow to the feet. This can make it difficult to feel any pain or discomfort, such as feeling pressure from a tight shoe, a cut, or an object in a shoe. An undetected foreign object in a shoe can lead to a blister or a sore which can then lead to an infection, poor healing, and, in some cases, amputation. (5)
Gangrene is a serious foot complication related to diabetes. Dead tissue appears on the tips of the toes as blackened areas of the skin. It can spread to the entire toe, surrounding toes, and the entire foot, which then can require amputation. Injuries of any kind – especially on the feet – are concerning for people with diabetes. Even a small cut can produce serious consequences for a person with diabetes as it increases the risk of fungal infections, bunions, and ulcers which can lead to a skin or bone infection. Fortunately, these complications can be prevented with proper foot care and controlling diabetes glucose levels. Any pain or discomfort to the feet should not be ignored. (6)
Anyone with diabetes can develop neuropathy. Diabetic neuropathy may affect as many as 50% of people with diabetes. The following are risk factors that can cause nerve damage:
- Poor blood sugar control. Uncontrolled blood sugar puts you at risk of every diabetes complication, including nerve damage.
- Diabetes history. Your risk of diabetic neuropathy increases the longer you have diabetes, especially if your blood sugar isn’t well controlled.
- Kidney disease. Diabetes can damage the kidneys. Kidney damage sends toxins into the blood, which can lead to nerve damage.
- Being overweight. Having a body mass index (BMI) of 25 or more may increase your risk of diabetic neuropathy.
- Smoking narrows and hardens your arteries, reducing blood flow to your legs and feet. This makes it more difficult for wounds to heal and damages the peripheral nerves.
To avoid serious foot problems that could result in losing a toe, foot, or leg, follow these guidelines when practicing foot care.
- Inspect your feet daily. Check for cuts, blisters, redness, swelling, or nail problems. Use a magnifying hand mirror to look at the bottom of your feet. Call your doctor if you notice anything.
- Bathe feet in lukewarm (never hot) water. Keep your feet clean by washing them daily. Use only lukewarm water—the temperature you would use on a newborn baby.
- Be gentle when bathing your feet. Wash them using a soft washcloth or sponge. Dry by blotting or patting, drying carefully between the toes.
- Moisturize your feet but not between your toes. Use a moisturizer daily to keep dry skin from itching or cracking. But don’t moisturize between the toes—that could encourage a fungal infection.
- Cut nails carefully. Cut them straight across and file the edges. Don’t cut nails too short, as this could lead to ingrown toenails. If you have concerns about your nails, consult your doctor.
- Never treat corns or calluses yourself.No “bathroom surgery” or medicated pads. Visit your doctor for appropriate treatment.
- Wear clean, dry socks. Change them daily.
- Consider socks made specifically for patients living with diabetes. These socks have extra cushioning, do not have elastic tops, are higher than the ankle, and are made from fibers that wick moisture away from the skin.
- Wear socks to bed. If your feet get cold at night, wear socks. Never use a heating pad or a hot water bottle.
- Shake out your shoes and feel the inside before wearing them. Remember, your feet may not be able to feel a pebble or other foreign object, so always inspect your shoes before putting them on.
- Keep your feet warm and dry. Don’t let your feet get wet in snow or rain. Wear warm socks and shoes in winter.
- Consider using an antiperspirant on the soles of your feet. This is helpful if you have excessive sweating of the feet.
- Never walk barefoot. Not even at home! Always wear shoes or slippers. You could step on something and get a scratch or cut.
- Take care of your diabetes. Keep your blood sugar levels under control.
- Do not smoke. Smoking restricts blood flow in your feet.
- Get periodic foot exams. Seeing your foot and ankle surgeon on a regular basis can help prevent the foot complications of diabetes. (5)
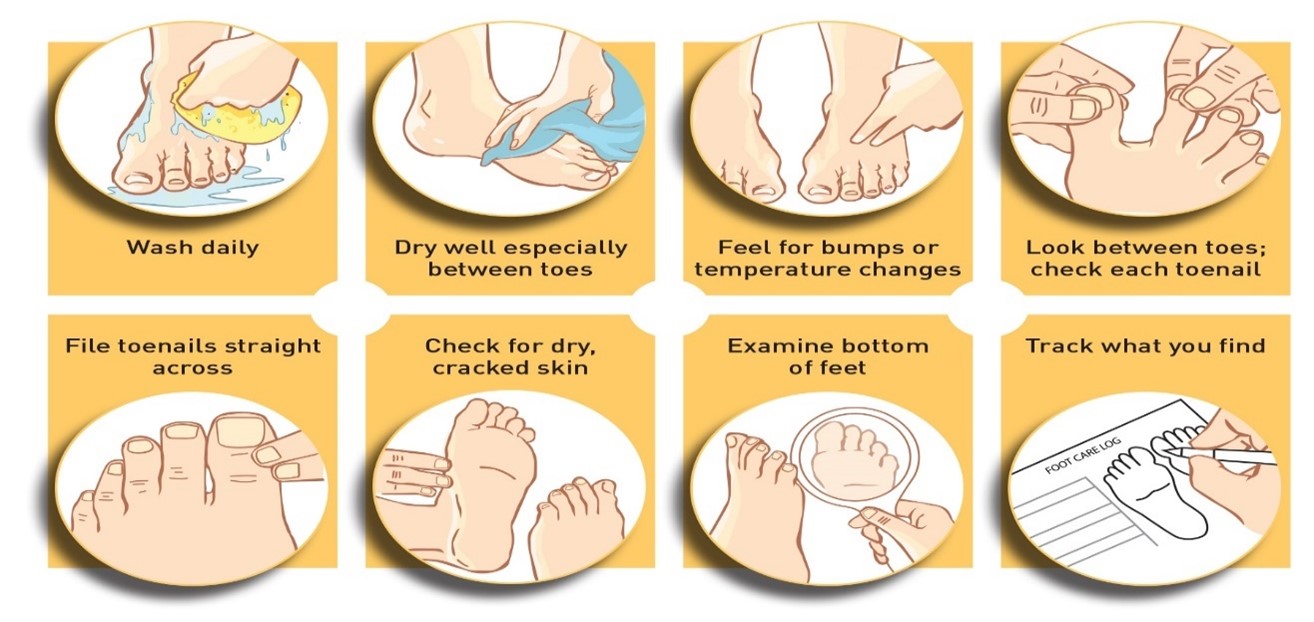
It is important to follow up with your healthcare provider regularly or as advised and report any injury to the feet. (i.e., cut, puncture, scrape, blister, bunion, hammertoes, ingrown toenail, or ulcer). (6)
CHW and Their Work in Addressing Diabetes
Community Health Workers are trusted members of the community and work in both clinical and non-clinical settings. Community Health Workers (CHWs) provide the community with health education and referrals to health and social services. CHWs meet participants where they are and know how to find hard-to-reach Hispanic/Latino participants as they are from the same community they serve. CHWs can address diabetes within their communities as they can speak the same language and take the time to meet with participants and their families. While their primary role is often linking vulnerable populations to the health system, CHWs may assist in other roles. These can range from cultural mediation, culturally appropriate education, care coordination, case management, systems navigation, coaching and social support, advocacy, capacity building, and outreach. Through these roles, CHWs offer support to patients with diabetes and those at risk of developing diabetes in a unique, culturally appropriate manner. (7)
The Role of CHWs in Supporting Diabetes Management
CHWs use a participant-centered approach that provides education, support, and skill-building to help participants live healthier lives. For example, CHWs at MHP Salud enroll program participants via door-to-door outreach in predominantly Latino and Hispanic neighborhoods. Participants are screened for their risk of diabetes and then enrolled in disease self-management education classes led by CHWs. These classes consist of six weekly sessions during which participants learn how to manage chronic diabetic kidney disease. Throughout the classes, CHWs share practical tips, suggestions, and strategies to build confidence in managing chronic illness and symptoms, such as fatigue, pain, shortness of breath, disability, and depression. The six sessions consist of the following topics: Diabetes and Hypertension, Healthy Eating, Recipes, Physical Activity, and its Benefits, Stress Management, and Relapse. Participants will have their blood pressure, weight, and BMI calculated at session one and then again at session six. (7)
CHWs promote action planning and goal-setting techniques to help participants achieve a healthier lifestyle. Upon completion, CHWs follow up with participants to ensure they have access to the resources they need (i.e., medical assistance programs, health insurance, and specialist visits). MHP Salud’s CHWs also encourage participants to incorporate program topics into their daily life. (7)
I take pride in my work as a Community Health Worker. I see the change and growth in my participants after they attend our sessions on diabetes management. CHWs take the time to go over details of their diagnosis such as what foods we can replace on our healthy plates, medicine storage, physical activity, and self-care to include stress management, attending doctors’ appointments, and follow-ups. In our sessions, we go over foot care with our participants and show them models of foot injuries to give them an idea of what to look out for. It’s all in the details, as we explain to our participants in our sessions. For example, we can suggest wearing white socks to our participants with nerve damage so they can notice any blood stains which can be a result of a foreign object in a shoe they didn’t feel throughout the day. We suggest filing their nails versus cutting their nails, passing a mirror under their feet, or having someone else check under their feet for any injury. We always think the worst complications will not happen to us, but nerve damage and amputations are a reality for patients with diabetes. We encourage our participants to take time for their care and make small, long-lasting changes.
Join Us and Other Professionals During Our Free Techincal Assistance Calls
Our Capacity Assistance Building team regularly holds technical assistance and webinars to support your programs. Click here to learn more!
- http://www.ncfh.org/diabetes-fact-sheet.html
- https://www.cdc.gov/diabetes/library/features/hispanic-diabetes.html
- https://aftagriculturaltourism.com.au/foot-care-tips-farmers-feet-injury-free
- https://www.mayoclinic.org/diseases-conditions/diabetic-neuropathy/symptoms-causes/syc-20371580
- https://www.foothealthfacts.org/conditions/diabetic-foot-care-guidelines
- https://www.crh.org/healthy-tomorrow/healthy-tomorrow/2018/10/24/diabetic-foot-care
- https://mhpsalud.org/community-health-worker-resources/community-health-workers-diabetes/
This publication is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award totaling $687,959.00 with 0 percentage financed with non-governmental sources. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS or the U.S. Government. For more information, please visitwww.HRSA.gov.
Blog Topics

This guide will provide access to information that will facilitate the identification of CHWs in their Health Centers and their roles in addressing diabetes self-management and prevention in their communities.