Diabetes Management and Oral Health
Published March 2022 | Back to all news and updates.
Migrant Seasonal Agricultural Workers (MSAWs) are predominantly Latino/Hispanic, and diabetes is most prevalent among the Latino/Hispanic communities. MSAWs frequently travel for work, leading to the lack of health insurance in their new state. Most MSAWs have poor general health and are working and living with chronic illnesses such as type II diabetes. The harsh working conditions can place MSAWs at higher risk for health complications as they are most likely to skip meals and take medication at prescribed times when working long shifts.1 Besides lack of health insurance, linguistic barriers, and lack of time for general medical care, MSAWs face a lack of dental insurance and dental care, which can lead to deteriorating oral health. Dental disease is one of the most common and preventable diseases but is not always the priority of patients managing diabetes.6
Diabetes management can be a daily struggle requiring a balance of nutrients, exercise, and medication. Uncontrolled diabetes can lead to many complications on the body, such as amputations, nerve damage, and vision loss, to name a few. Diabetes can also affect oral health. If you live with diabetes, it is essential to pay particular attention to your oral health and dental care and keep your blood glucose levels in the target range. Having high or irregular blood glucose levels can lead to gum disease and loss of teeth.1
Having uncontrolled diabetes can lead to dry mouth decreasing saliva flow which can cause soreness, ulcers, infections, and tooth decay. Oral health is crucial as it relates to diabetes because high blood sugar can also weaken white blood cells, which is the body’s primary way of fighting infections.2 Besides weakening white blood cells, diabetes can cause blood vessels to thicken, slowing down the blood flow to tissues in the body, leading to poor healing causing infections, gum inflammation (gingivitis), bleeding of the gums, and periodontitis.3
Managing blood sugar levels is critical. The higher your blood sugar level, the higher your risk of:
- Tooth decay (cavities). Your mouth naturally contains many types of bacteria. When starches and sugars in foods and beverages interact with these bacteria, a sticky film known as plaque forms on your teeth. The acids in plaque attack the surfaces of your teeth (enamel and dentin). This can lead to cavities and gum disease.
The higher your blood sugar level, the greater the supply of sugars and starches, causing more acid wearing at your teeth.
- Early gum disease (gingivitis). Diabetes reduces your ability to fight bacteria. If you don’t remove plaque with regular brushing and flossing, it’ll harden under your gumline into a substance called tartar (dental calculus).
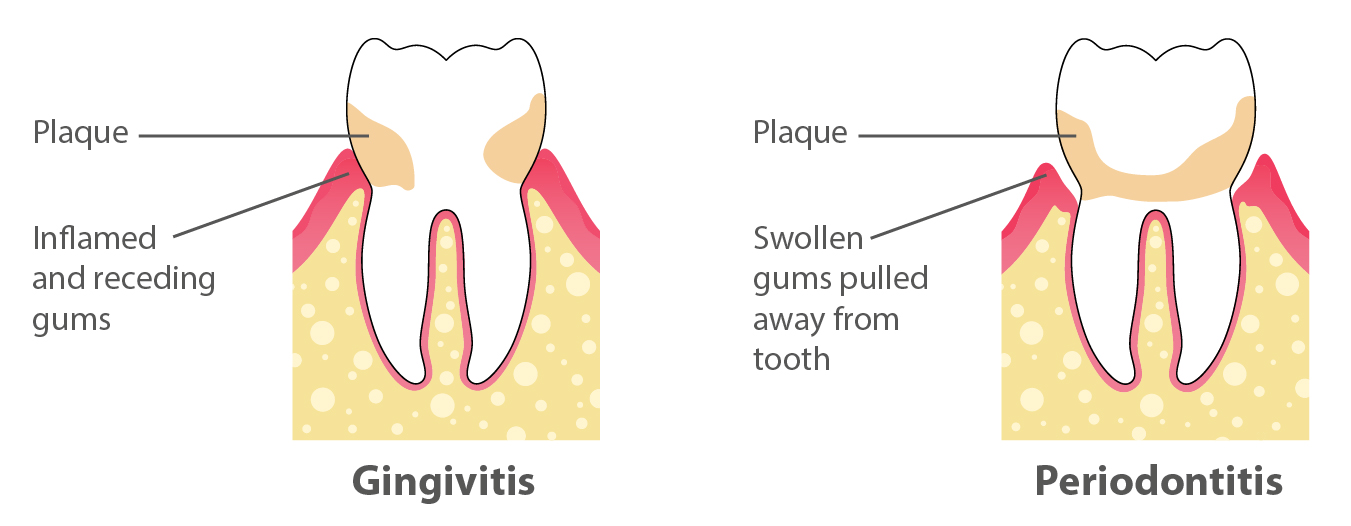
The longer plaque and tartar remain on your teeth, the more they irritate the part of your gums around the base of your teeth, called the gingiva. In time, your gums become swollen and bleed easily; this is known as gingivitis.
- Advanced gum disease (periodontitis). If left untreated, gingivitis can lead to a more severe infection called periodontitis, which destroys the soft tissue and bone that support your teeth. Eventually, periodontitis causes your gums and jawbone to pull away from your teeth, which in turn causes your teeth to loosen and possibly fall out.
Periodontitis tends to be more severe among people with diabetes because the disease lowers the ability to resist infection and slows healing. A condition such as periodontitis may also cause your blood sugar level to rise, making your diabetes more difficult to control. Preventing and treating periodontitis with regular dental cleanings can help improve blood sugar control.
- People with diabetes may be more likely to develop thrush, a fungal infection caused by candida albicans (a type of yeast). Signs of thrush include painful white or red patches inside your mouth. Practicing good oral hygiene can help you avoid thrush.
Dry mouth (xerostomia). Some people with diabetes also experience a lack of saliva, a condition known as dry mouth. Without saliva to keep your mouth moist and bathe your teeth, you could be at risk of tooth decay, gum disease, and thrush.4
Prevention
Diabetes management is vital to prevent complications related to this chronic disease’s effects on oral health. Complications to the gums and teeth can be prevented by keeping blood sugar levels in check, taking medications as prescribed, and attending dental visits every 6 to 12 months or as directed by a health professional. Other measures to prevent complications are to floss daily, brush teeth after every meal with a soft bristle toothbrush, rinse mouth with mouthwash, clean dentures daily, and refrain from smoking.5 Always inform your dentist of swollen gums or any discomfort.
CHW and Their Work in Addressing Diabetes
A Community Health Worker (CHW) is a trusted member of the community they serve. CHWs work in clinical and non-clinical settings and provide health education and referrals to local organizations that assist with health and social services. CHWs meet participants where they are – at home, at work, or out in the community – to better reach participants and meet their unique needs. CHWs are often bilingual, which helps to better connect and communicate with MSAW communities. While their primary role is often linking vulnerable populations to the health system, additional roles can include cultural mediation, culturally appropriate education, care coordination, case management, systems navigation, coaching and social support, advocacy, capacity building, and outreach. Through these roles, CHWs offer support to participants with diabetes and/or at risk of developing diabetes in a unique, culturally appropriate manner. Due to their intimate understanding of and trust from the community they serve, CHWs have a unique ability to build strong relationships and effectively address challenges individuals face when trying to manage chronic conditions such as diabetes. CHWs also conduct home visits and speak one-on-one with participants on the importance of proper nutrition, physical exercise, and disease management. Overall, CHW interventions have successfully improved health outcomes among individuals diagnosed with diabetes and supported at-risk individuals to prevent the development of the condition.6
MHP Salud’s CHW Diabetes Programs
MHP Salud’s diabetes programs provide accessible support and education to vulnerable populations so they can live healthier lives. These programs focus on community-based educational classes led by a CHW, either in person or virtually, to provide educational instruction on how participants can understand their diagnosis, manage their diabetes, and maintain a healthy lifestyle. CHWs culturally identify with program participants and provide appropriate recommendations that participants will be receptive to based on their available resources.
Juntos Podemos (Together We Can!) is a healthy lifestyle program led by CHWs in South Texas. Juntos Podemos is an example of a family-centered, CHW-led intervention that educates families on the importance of healthy lifestyle behaviors to reduce risk factors for diabetes. This program supports Latino families on federal assistance programs, like the Supplemental Nutrition Assistance Program (SNAP). The program’s goal is to promote the adoption of healthy lifestyle behaviors by educating families on better nutrition and exercise habits. The program consists of four 90-minute health education classes led by CHWs using the National Institute of Health’s We Can! (Ways to Enhance Children’s Activity Nutrition) curriculum. This research-based curriculum gives parents/caregivers and entire communities tangible tools to help them engage and educate their families on healthy behaviors. The curriculum provides bilingual (English and Spanish) information and educational resources.6
“I feel that the work I do as a Community Health Worker is very important in the lives of my participants. I listen to my participants, their concerns, and any worries they may have. I can refer them to local services such as food banks, utility assistance, and health services or education services which help them better their lives overall. Some of our participants do not have health insurance (i.e., unemployed or are not U.S. Citizens), and we can refer them to mobile clinics, non-profit clinics, or local services that provide oral health such as free dentist visits or low-cost services. These services allow our participants to get free or low-cost dental evaluations, checkups, and orthodontic services as needed. It is most satisfying to see how grateful participants are to receive these services.”
Mary Zepeda, MHP Salud Community Health Worker
Diabetes Resources:
Center for Disease Control
The Center for Disease Control (CDC) website shares Tips to Keep Your Teeth Health, an online resource to take charge of your diabetes and keep your teeth healthy. The resource shares how diabetes can harm teeth and the signs of gum disease. To read on managing your diabetes and oral health, click here.
Diabetes: Dental Tips
The National Institute of Dental and Craniofacial Research share their online resource on Diabetes: Dental Tips. This resource includes steps to keeping your mouth healthy while managing diabetes. To read more, click here.
Academy of General Dentistry
The Academy of General Dentistry article on Oral Health and Diabetes includes how oral health problems are associated with diabetes, the symptoms to be aware of, and how to prevent dental complications related to diabetes. To read more, click here.
Better Health Channel
The Better Health Channel shares a Diabetes and Healthy Eating video and tips on how to manage diabetes by eating healthier, portion sizes, physical activity, and overall care. To read more and to watch the video, click here.
Want to learn more about our diabetes prevention and management initiatives? Click here!
- https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/diabetes-and-oral-health
- https://www.cdc.gov/diabetes/managing/diabetes-oral-health.html
- https://my.clevelandclinic.org/health/diseases/11263-oral-health-problems-and-diabetes
- https://www.mayoclinic.org/diseases-conditions/diabetes/in-depth/diabetes/art-20043848
- https://www.webmd.com/diabetes/diabetes-affects-teeth
- http://www.ncfh.org/oral-health.html
This publication is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award totaling $678,959.00 with 0 percentage financed with non-governmental sources. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit www.HRSA.gov.
Blog Topics
This resource provides educational tools that Community Health Workers (CHWs) can use and share with Migrant Seasonal Agricultural Workers and other vulnerable populations to reduce diabetic health complications in oral, eye, and foot health, which are commonly linked to diabetes.